Goal Four: Increase Efficiency, Transparency, and Accountability of HHS Programs
Reducing the Reporting Time for Pediatric Cancer Cases
CDC completed implementation of early case capture (ECC) for pediatric cancer patients in seven central cancer registries. As a result, 97 percent of ECC cases are now reported within nine months to the central cancer registry and are available for research use and incidence reporting at the state level, less than half the time it takes for routine reporting (18-24 months).
As the largest grant-awarding agency in the Federal Government and the nation’s largest health insurer, HHS places a high priority on ensuring the integrity of its expenditures. HHS manages hundreds of programs in basic and applied science, public health, income support, child development, and health and social services, which award over 75,000 grants annually. The Department has robust processes in place to manage the resources and information employed to support programs and activities.
Goal Four includes four objectives:
- Strengthen program integrity and responsible stewardship by reducing improper payments, fighting fraud, and integrating financial, performance, and risk management
- Enhance access to and use of data to improve HHS programs and to support improvements in the health and well-being of the American People
- Invest in the HHS workforce to help meet America’s health and human services needs
- Improve HHS environmental, energy, and economic performance to promote sustainability
For the past two years, AHRQ’s Consumer Assessment of Healthcare Providers and Systems (CAHPS) team has been working with the Center for Consumer Information and Insurance Oversight at CMS to develop a CAHPS Survey called the Quality Health Plan Enrollee Survey. In 2015, the Quality Health Plan Enrollee Survey will be administered to a sample of enrollees in qualified health plans participating in the Health Insurance Marketplaces established by the Affordable Care Act. This information will ultimately be published on Healthcare.gov for the 2017 plan year and will allow consumers to review assessments of enrollee satisfaction as part of their plan selection process, thus allowing them to choose the best plan for the needs of themselves and their families.
A foundation of ACL’s program success is access to Home and Community-based Services. In FY 2013, the Aging Services Network served 9,753 clients per million dollars of Older Americans Act funding, exceeding the target of 8,700. This reflects the success of ongoing initiatives to improve program management and expand options for home and community-based care. Aging and Disability Resource Centers, along with increased commitments and partnerships at the state and local levels, have all had positive impacts on program efficiency. Between FY 2007 and FY 2013 performance has improved by nearly 17 percent, without the benefit of adjustment for inflation.
 One of CMS’ key goals is to pay claims properly the first time. This means paying the right amount, to legitimate providers, for covered, reasonable and necessary services provided to eligible beneficiaries. Paying correctly the first time saves resources required to recover improper payments and ensures the proper expenditure of valuable Medicare Trust Fund dollars. The Medicare Fee-for-Service (FFS) improper payment estimate is calculated under the Comprehensive Error Rate Testing (CERT) Program. CMS did not meet the 2014 target for this measure, reporting an FY 2014 Medicare FFS improper payment rate of 12.7 percent, falling short of the 9.9 percent target. The primary causes of improper payments were due to Administrative and Documentation errors, in large part due to insufficient documentation. CMS has already taken several steps to correct these errors, including modifying the Home Health regulations to improve documentation of the face-to-face requirement and implementing new prior authorization demonstrations to improve quality and reduce improper payments.
One of CMS’ key goals is to pay claims properly the first time. This means paying the right amount, to legitimate providers, for covered, reasonable and necessary services provided to eligible beneficiaries. Paying correctly the first time saves resources required to recover improper payments and ensures the proper expenditure of valuable Medicare Trust Fund dollars. The Medicare Fee-for-Service (FFS) improper payment estimate is calculated under the Comprehensive Error Rate Testing (CERT) Program. CMS did not meet the 2014 target for this measure, reporting an FY 2014 Medicare FFS improper payment rate of 12.7 percent, falling short of the 9.9 percent target. The primary causes of improper payments were due to Administrative and Documentation errors, in large part due to insufficient documentation. CMS has already taken several steps to correct these errors, including modifying the Home Health regulations to improve documentation of the face-to-face requirement and implementing new prior authorization demonstrations to improve quality and reduce improper payments.
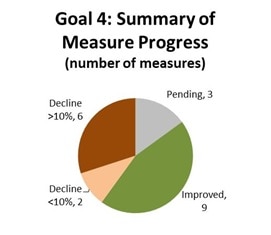
For this goal, 53 percent of measures with available data showed stable or improved performance.
